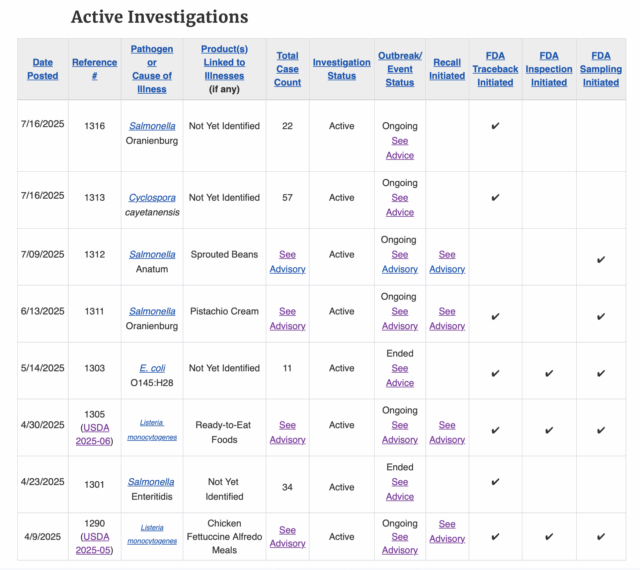
- For the outbreak of Salmonella Oranienburg (ref #1316) linked to a not yet identified product, FDA has initiated traceback. The case count has increased from 18 to 22.
- For the outbreak of Cyclospora cayetanensis (ref #1313) linked to a not yet identified product, an additional cluster of Cyclosporiasis illnesses has been added to this investigation based on data provided by Centers for Disease Control and Prevention. The case count has been adjusted from 24 to 57.
- For the outbreak of Salmonella Anatum (ref #1312), Chetak LLC Group has issued a recall of Deep-brand frozen sprouted mat (moth) and moong (mung) beans. FDA has issued an advisory with additional product information.
- For the outbreak of Salmonella Oranienburg (ref #1311) linked to pistachio cream, FDA updated the advisory to include a recall. See the advisory for product information.
- For the outbreak of hepatitis A virus (ref #1302) linked to a not identified product, the outbreak has ended, and FDA’s investigation is closed.